FAQs on Pelvic Pain
Pelvic pain is a common condition among women. The nature and intensity of pelvic pain can fluctuate, and the cause of pelvic pain is often unknown. For some women, there is no evident disease.
Pelvic pain is categorized as acute (sudden and short-term) or chronic (persistent and long-standing). Pelvic pain can be related to the reproductive organs in the pelvis, or it can be related to the gastrointestinal tract.
What causes pelvic pain?
Pelvic myofascial pain is often a consequence of effects on neural or connective tissue changes, which arise from injury or trauma. The pelvic floor musculature is sometimes a source of pelvic pain as well. Pelvic pain could be related to:
- Irritation of nerves or inflammation caused by fibrosis, injury, pressure, or infection
- Contraindications and/or cramps of skeletal and smooth muscles
- Ectopic pregnancy
- Ruptured or twisted ovarian cyst
- Pelvic inflammatory disease/scarring
- Endometriosis
- Uterine fibroids and endometrial polyps
What are the types of pelvic pain?
The types of pelvic pain depend on the origin or cause. These include:
- Localized pain – Usually due to inflammation or infection.
- Cramping – Caused by spasm of soft tissue/organs.
- Onset of pain – Sudden onset is usually due to obstruction of blood flow. Gradual onset can be from appendix inflammation or intestinal obstruction.
- Aggravated by movement – When pain is worse during movement, it could be from irritation to the abdominal cavity lining.
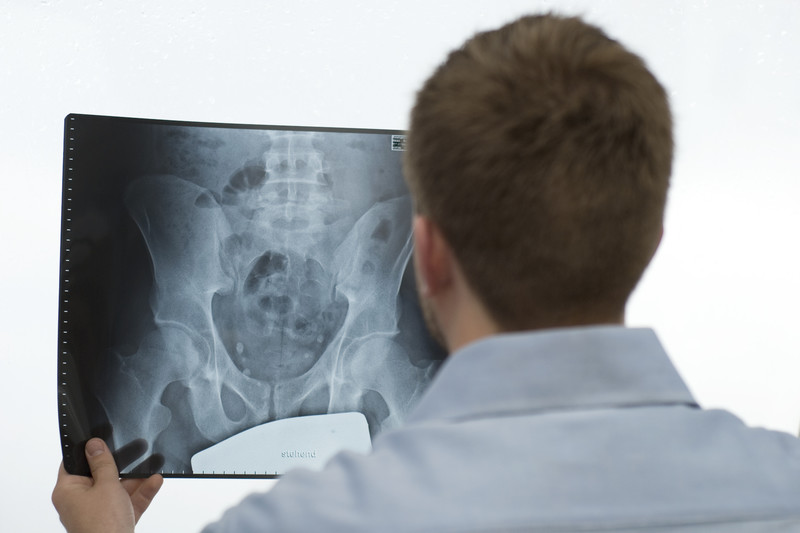
How is pelvic pain diagnosed?
When you see a pain management specialist about your pelvic pain, the healthcare provider will take a detailed medical history. During your consultation, the doctor will conduct a comprehensive physical examination, which includes a pelvic exam. It is necessary for the doctor to find the cause of your pain. Tests used to diagnose pelvic pain include ultrasound, laparoscopy, cystoscopy, colonoscopy, and sigmoidoscopy.
What are some of the treatments for chronic pelvic pain?
Some of the treatment options for chronic pelvic pain include:
- Physical therapy – Acupressure, ultrasound therapy, and electrical stimulation are some of the therapies used for treating pelvic pain.
 These treatments ease trigger points and give relief to muscle discomfort.
These treatments ease trigger points and give relief to muscle discomfort. - Lifestyle changes – Regular exercise and good posture can reduce pain.
- Medications – Nonsteroidal anti-inflammatory drugs are used to reduce the pain associated with inflammation and cramps.
- Trigger point injections – Myofascial trigger points can give rise to pelvic pain. These points serve as triggers for pain and are palpable as band-like prominences in the muscle belly. Trigger point injections reverse the cycle of spasm. This involves injecting lidocaine or Botox into these trigger points to deactivate them.
- Nerve block – Fluroscopically-guided interventions are used to inject a blocking agent (lidocaine or phenol) onto a nerve that supplies the pelvic region. This is done under twilight anesthesia and sterile technique. The targeted nerves are the superior hypogastric plexus and the ganglion impar.
Does stem cell therapy help pelvic pain?
In a study from the University of California, researchers used stem cells in rat subjects with spinal cord injury. After stem cell implantation, the subjects experienced improvements in both motor function and sensory function. The authors also noted that the stem cells prevented cavity formation.
There have been two groundbreaking studies evaluating stem cell therapy for pelvic pain, specifically pudendal neuralgia. The first study in 2015 involved fifteen patients and entailed injections around the pudendal nerve. Of the 12 who completed the study, 10 had amazing improvements in their pain. A follow up study in 2017 by Jarnagin et al included sixty four patients and was published din the Journal of Minimally Invasive Gynecology. The study, titled Resolution of Pudendal Neuralgia in Chronic Pelvic Pain, found that 90% of the patients received moderate or complete relief of pain. There were no complications.
Amniotic fluid is a great source of stem cells, and it is donated after C-section by women. The fluid contains growth factors, hyaluronic acid, and anti-inflammatory agents that work to reduce pelvic pain. A recent study found that stem cells were useful for reducing inflammation in knee arthritis.
Resources
Braz JM, Sharif-Naeini R, Vogt D, Kriegstein A, Alvarez-Buylla A, Rubenstien JL, Basbaum AI: Forebrain GABAergic neuron precursors integrate into adult spinal cord and reduce injury-induced neuropathic pain. Neuron 2012; 74:663-75.
Jergova S, Hentall ID, Gajavelli S, Varghese MS, Sagen J: Instraspinal transplantation of GABAergic neural progenitors attenuates neuropathic pain in rats: a pharmacologic and neurophysiological evaluation. Exp Neurol 2012; 234:39-49.
Jarnagin et al, Resolution of Pudendal Neuralgia in Chronic Pelvic Pain, Journal of Minimally Invasive Gynecology, Volume 24, Issue 7, Supplement, November–December 2017, Pages S185–S186.
Venturi et al, Pudendal Neuralgia: A New Option for Treatment, Pain Medicine 2015: 16: 1475-1481.